Overview
Psoriasis is a chronic autoimmune skin condition that speeds up the life cycle of skin cells, causing them to build up rapidly on the surface. This leads to red, scaly, itchy patches that can be uncomfortable and sometimes painful. While it primarily affects the skin, psoriasis is not just “skin deep.” It is linked to other health problems such as psoriatic arthritis, cardiovascular disease, and depression.
Globally, psoriasis affects about 2–3% of the population, including millions of people who struggle daily with both physical and emotional challenges. Raising awareness is key to reducing stigma, improving access to care, and helping people understand that psoriasis is a manageable medical condition—not a contagious skin disease.
Key Awareness Points You Should Know!
It’s common but misunderstood: Many assume psoriasis is caused by poor hygiene—it’s not. It is an immune-related condition.
Different types exist: Plaque psoriasis is the most common, but there are others (guttate, pustular, inverse, erythrodermic).
It affects more than skin: Up to 1 in 3 people with psoriasis may develop psoriatic arthritis, which causes painful joint inflammation.
Psychological impact is real: Stigma, embarrassment, and visible skin changes often affect self-esteem and mental health.
Management Tips
1. Medical Treatments
Topical treatments: Creams and ointments like corticosteroids or vitamin D analogues help mild to moderate cases.
Phototherapy: Controlled UV light treatment can reduce flare-ups.
Systemic medications: For moderate to severe psoriasis, oral or injectable medications (such as methotrexate, cyclosporine, or biologics) target the immune system.
New therapies: Recently approved medications such as deucravacitinib (Sotyktu) and tapinarof (Vtama) offer new hope for people not responding to older treatments.
N/B: Always consult a dermatologist before starting or changing treatment.
2. Lifestyle & Self-Care
Moisturize daily: Prevents dryness and reduces scaling.
Avoid triggers: Stress, skin injuries, infections, smoking, and alcohol can worsen psoriasis.
Healthy diet: A balanced, anti-inflammatory diet (like the Mediterranean diet) may help reduce flare severity.
Stay active & maintain a healthy weight: Reduces inflammation and improves treatment response.
Protect your mental health: Counseling, support groups, and stress-reducing activities like yoga or meditation are beneficial.
3. Working With Your Care Team
Dermatologists: For diagnosis and treatment planning.
Rheumatologists: If joint pain suggests psoriatic arthritis.
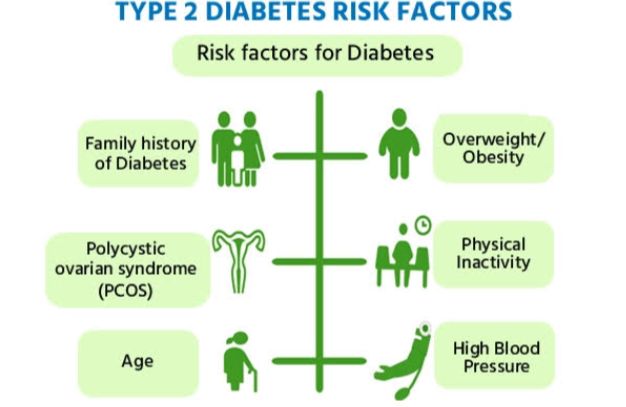
Primary care providers: To manage comorbid conditions like heart disease or diabetes.
Mental health support: Addressing the emotional burden of psoriasis is just as important as treating the skin.
Breaking the Stigma
One of the biggest challenges for people with psoriasis is misconception and stigma.
Psoriasis is not contagious, and with proper treatment, individuals can live normal, healthy lives.
NOTE: Psoriasis may be a lifelong condition, but with the right treatment, lifestyle adjustments, and support, symptoms can be controlled, flares minimized, and quality of life improved.